Abstracts of the 13th International Conference on Thrombosis and Hemostasis Issues in Cancer, 2026
Vol. 5 No. s1 (2026)
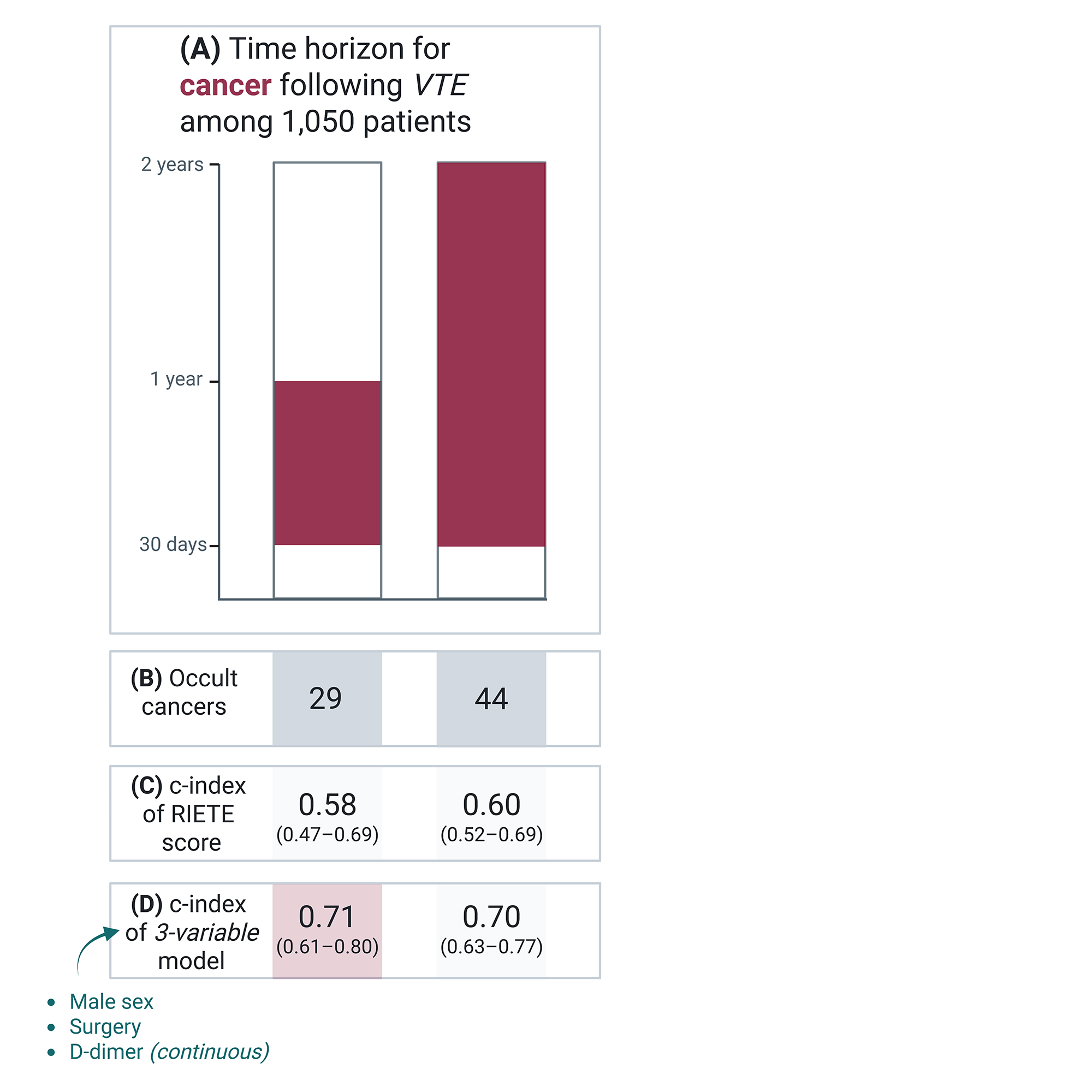
PO57 | A NOVEL RISK ASSESSMENT MODEL FOR CANCER DETECTION WITHIN ONE YEAR AFTER INCIDENT VENOUS THROMBOEMBOLISM
C. Antoun1, J. Hansen1|3, S. Brækkan1|3, C. Langholm1, N. Eide1, V. Morelli1|3, K. Hveem2 | 1Department of Clinical Medicine, UiT The Arctic University of Norway, Tromsø; 2HUNT Center for Molecular and Clinical Epidemiology, Norwegian University of Science and Technology, Trondheim; 3Thrombosis Research Center, Division of Internal Medicine, University Hospital of North Norway, Tromsø, Norway

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 16 April 2026
1
Views
0
Downloads
Most read articles by the same author(s)
- Società Italiana di Emostasi e Trombosi, OC02 | INCIDENCE AND PREDICTORS OF ARTERIAL THROMBOSIS IN CANCER PATIENTS: RESULTS FROM THE PROSPECTIVE COMPASS-ARTERIAL CANCER ASSOCIATED THROMBOSIS (COMPASS-ARTECAT) STUDY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, OC04 | DIRECT ORAL ANTICOAGULANTS PROVIDE EFFECTIVE THROMBOPROPHYLAXIS IN NEWLY DIAGNOSED MYELOMA: REAL WORLD FINDINGS FROM THE ATOMM STUDY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO56 | EXTERNAL VALIDATION OF THE SAVED SCORE IN A CANADIAN REGIONAL CANCER CENTER COHORT: A REAL-WORLD ANALYSIS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, OC08 | A SILK-BASED 3D BONE MARROW MODEL FOR CHEMOTHERAPY-INDUCED THROMBOCYTOPENIA , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO02 | SYNERGISTIC INTERACTION OF ENDOTHELIAL AND CANCER CELLS IN THE FORMATION AND STRUCTURE OF THE FIBRIN CLOT SHIELDS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO72 | CATHETER-RELATED THROMBOSIS VS. FIBROBLASTIC SLEEVE. INCIDENCE AND IMPACT IN ONCOLOGICAL AND HEMATOLOGICAL PATIENTS WITH PERIPHERALLY INSERTED CENTRAL CATHETER , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, OC03 | THROMBOEMBOLIC PREVALENCE IN MULTIPLE MYELOMA BEFORE AND AFTER THE INTRODUCTION OF DIRECT ORAL ANTICOAGULANTS: A LONGITUDINAL COHORT STUDY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO11 | THROMBOEMBOLIC EVENTS DURING PERIOPERATIVE THERAPY FOR RESECTABLE AND BORDERLINE RESECTABLE PANCREATIC CANCER IN THE PREOPANC-2 TRIAL , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO61 | RISK FACTORS FOR INTRACRANIAL HEMORRHAGE: AN UMBRELLA REVIEW TO INFORM MACHINE LEARNING PREDICTION MODELS IN GLIOMA PATIENTS RECEIVING ANTICOAGULATION , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO24 | WE ARE JUGGLING MANY POSSIBILITIES: HEALTHCARE PROFESSIONALS’ EXPERIENCES AND PERSPECTIVES ON INTERPRETATION OF PULMONARY EMBOLISM SIGNS AND SYMPTOMS IN PATIENTS WITH LUNG CANCER , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)