Proceedings of the 13th International Conference on Thrombosis and Hemostasis Issues in Cancer, 2026
Vol. 5 No. s1 (2026)
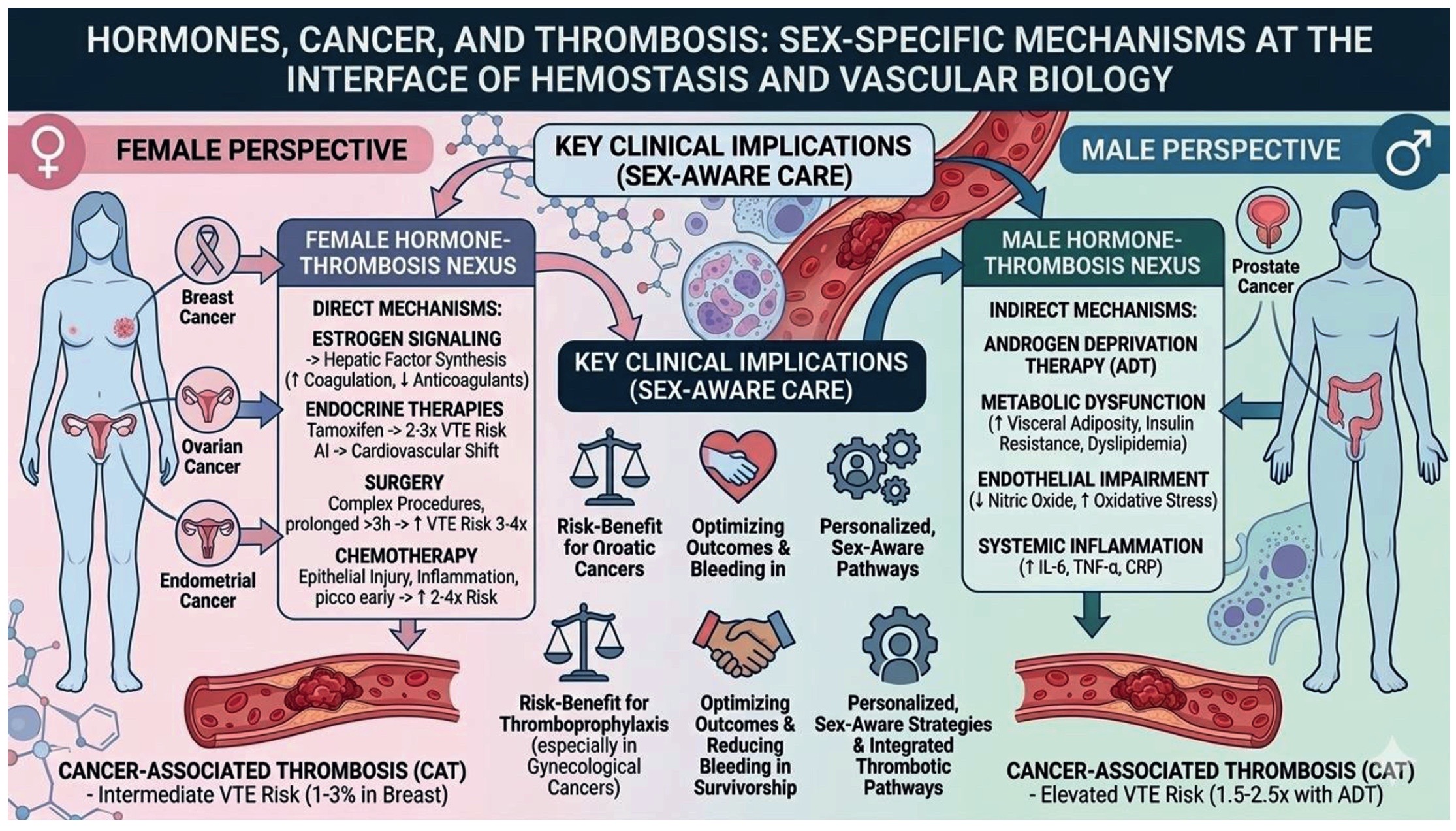
Hormones, cancer, and thrombosis: sex-specific mechanisms at the interface of hemostasis and vascular biology

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 16 April 2026
191
Views
115
Downloads
Most read articles by the same author(s)
- Roberto Mario Santi, Annamaria Fulghesu, Ezio Zanon, Erica De Candia, Elvira Grandone, Giancarlo Di Renzo, Claudia Succu, Valentina Tosto, Vincenzina Bruni, Paolo Gresele, Diagnosis and management of abnormal uterine bleeding in adolescence , Bleeding, Thrombosis and Vascular Biology: Vol. 3 No. 1 (2024)
- Giovanni L. Tiscia, Donatella Colaizzo, Antonio De Laurenzo, Filomena Cappucci, Lucia Fischetti, Elena Chinni, Mario Mastroianno, Giovanni Favuzzi, Massimo Carella, Elvira Grandone, Thrombin generation assay in COVID-19 patients shows a hypocoagulable pattern , Bleeding, Thrombosis and Vascular Biology: Vol. 3 No. 3 (2024)
- Giovanni Tiscia, Elvira Grandone, Talking about assisted reproductive techniques and thromboembolic risk: everything we always wanted to know , Bleeding, Thrombosis and Vascular Biology: Vol. 1 No. 2 (2022)
- Francesco Marongiu, Elvira Grandone, Silvia Marongiu, Antonella Mameli, Doris Barcellona, Stroke in women: anticoagulation in a complicated puzzle , Bleeding, Thrombosis and Vascular Biology: Vol. 3 No. 2 (2024)
- Daniela Poli, Riccardo Tartaglia, Doris Barcellona , Paolo Bucciarelli , Antonio Ciampa, Elvira Grandone, Giuseppe Malcangi, Giuseppe Rescigno, Vincenzo Toschi, Sophie Testa, Alessandro Squizzato, Attitude to clinical research among health professionals affiliated with the Italian Federation of Centers for the Diagnosis of Thrombotic Disorders and the Surveillance of the Antithrombotic Therapies (FCSA) , Bleeding, Thrombosis and Vascular Biology: Vol. 2 No. 1 (2023)