Reviews
Vol. 5 No. 1 (2026)
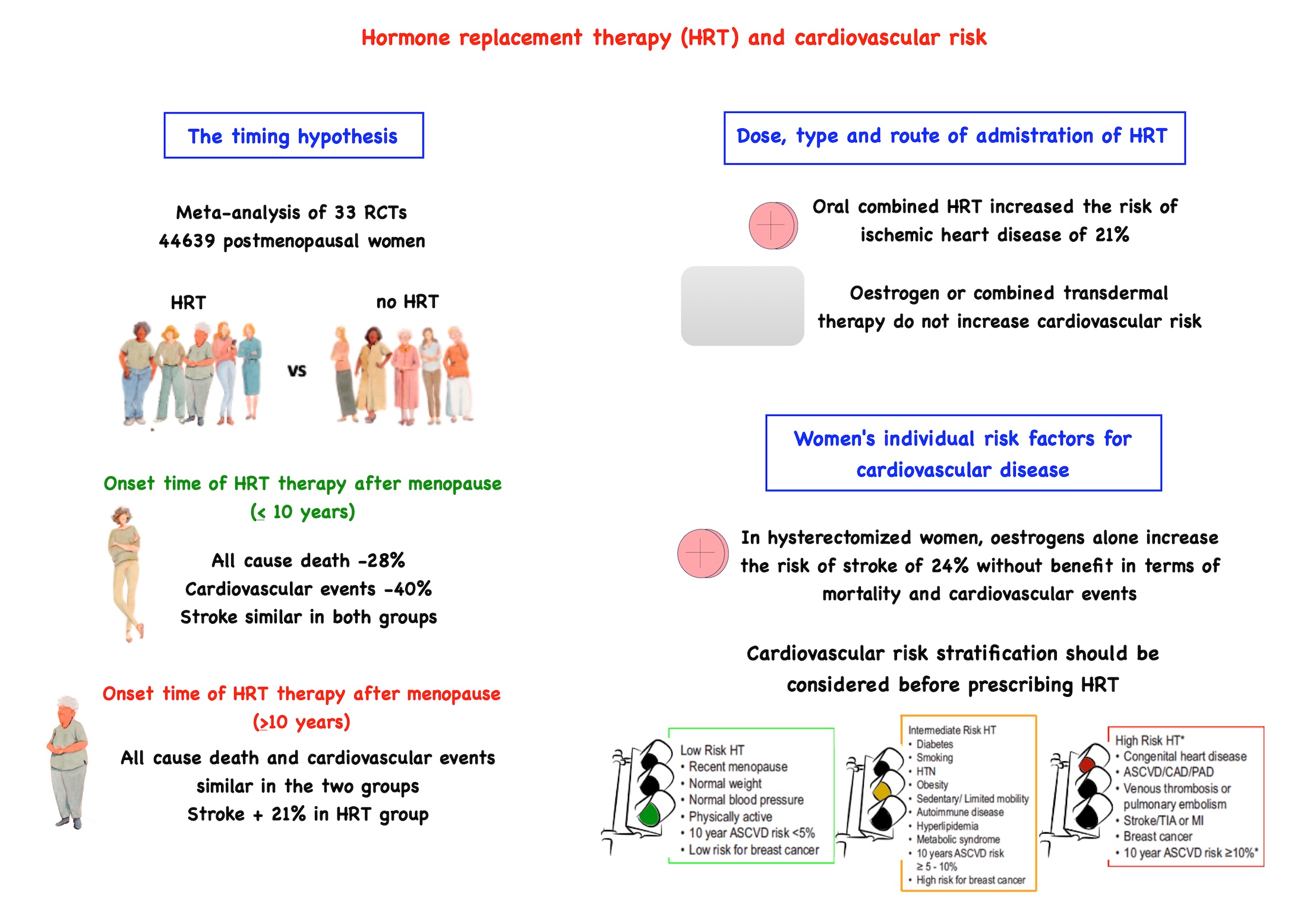
Cardiovascular risk in hormone replacement therapy

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 9 February 2026
1434
Views
259
Downloads
Most read articles by the same author(s)
- Francesco Marongiu, Elvira Grandone, Silvia Marongiu, Antonella Mameli, Doris Barcellona, Stroke in women: anticoagulation in a complicated puzzle , Bleeding, Thrombosis and Vascular Biology: Vol. 3 No. 2 (2024)
- Daniela Poli, Riccardo Tartaglia, Doris Barcellona , Paolo Bucciarelli , Antonio Ciampa, Elvira Grandone, Giuseppe Malcangi, Giuseppe Rescigno, Vincenzo Toschi, Sophie Testa, Alessandro Squizzato, Attitude to clinical research among health professionals affiliated with the Italian Federation of Centers for the Diagnosis of Thrombotic Disorders and the Surveillance of the Antithrombotic Therapies (FCSA) , Bleeding, Thrombosis and Vascular Biology: Vol. 2 No. 1 (2023)