Abstracts of the 13th International Conference on Thrombosis and Hemostasis Issues in Cancer, 2026
Vol. 5 No. s1 (2026)
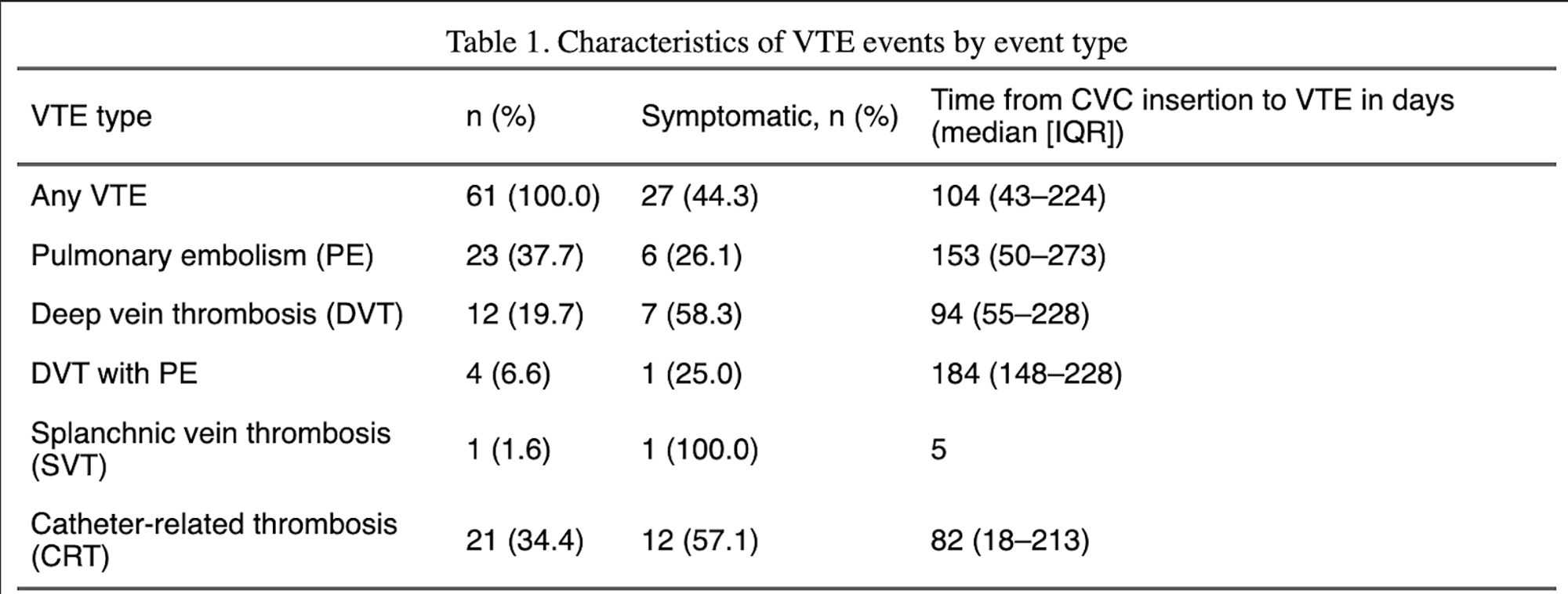
PO10 | RISK OF VENOUS THROMBOEMBOLISM IN CANCER PATIENTS WITH CENTRAL VENOUS CATHETERS: RESULTS FROM THE VIENNA CAT-BLED STUDY
B. Sunder-Plassmann 1, N, Vladic1, C. Englisch1, F. Moik1|3, V. Sunder-Plassmann2, A. Berghoff2, M. Preusser2, I. Pabinger1, C. Ay1 | 1Division of Hematology and Haemostaseology, Department of Medicine I, Medical University of Vienna; Vienna, Austria; 2Division of Oncology, Department of Medicine I, Medical University of Vienna; Vienna, Austria; 3Division of Oncology, Department of Internal Medicine, Medical University of Graz; Graz, Austria

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 16 April 2026
1
Views
0
Downloads
Most read articles by the same author(s)
- Società Italiana di Emostasi e Trombosi, OC05 | TIME TO START OF ANTICOAGULANT THERAPY AND SURVIVAL OUTCOMES IN CANCER PATIENTS WITH PULMONARY EMBOLISM , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO20 | DYSFUNCTION OF THE ADAMTS-13/VON WILLEBRAND FACTOR AXIS, MEDIATED BY NETOSIS, AS A DRIVER OF PROTHROMBOTIC STATE AND UNFAVORABLE PROGNOSIS IN ONCOGYNECOLOGICAL PATIENTS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO28 | CLINICAL IMPLICATIONS OF ANTICOAGULANT DRUG INTERACTIONS WITH TARGETED AND IMMUNE THERAPIES IN ONCOLOGY: A CONTEMPORARY RISK STRATIFICATION FRAMEWORK , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO37 | CLINICAL SIGNIFICANCE OF SYMPTOMATIC AND INCIDENTAL VENOUS THROMBOEMBOLISM IN CANCER PATIENTS TREATED WITH APIXABAN , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO57 | A NOVEL RISK ASSESSMENT MODEL FOR CANCER DETECTION WITHIN ONE YEAR AFTER INCIDENT VENOUS THROMBOEMBOLISM , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO03 | HEPATIC FIBROSIS–DRIVEN TISSUE FACTOR EXPRESSION BY MALIGNANT CHOLANGIOCYTES IS ASSOCIATED WITH CANCER-ASSOCIATED THROMBOSIS AND POOR SURVIVAL IN INTRAHEPATIC CHOLANGIOCARCINOMA , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO21 | PSYCHOLOGICAL IMPACT OF CANCER-ASSOCIATED THROMBOSIS: DUAL BURDEN AND IMPLICATIONS FOR QUALITY OF LIFE AND INTEGRATED PATIENT-CENTERED CARE , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO39 | RISK OF VENOUS THROMBOEMBOLISM ASSOCIATED WITH PERIPHERALLY INSERTED CENTRAL CATHETERS IN CANCER PATIENTS RECEIVING CHEMOTHERAPY: A REAL-WORLD SINGLE-CENTRE EXPERIENCE , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO50 | SUB-ANALYSIS OF INTERIM RESULTS FROM A PHASE 2 STUDY INVESTIGATING REGN9933A2 AND REGN7508CAT FOR THE PREVENTION OF CONTACT-MEDIATED VENOUS THROMBOEMBOLISM IN PATIENTS WITH ACTIVE CANCER UNDERGOING PERIPHERALLY INSERTED CENTRAL CATHETER PLACEMENT (ROXI-CATH) , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO58 | TACKLING THE AWARENESS GAP IN CANCER-ASSOCIATED THROMBOSIS: IMPACT OF A BRIEF EDUCATIONAL INTERVENTION IN PATIENTS WITH GYNECOLOGICAL CANCERS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)