Abstracts of the 13th International Conference on Thrombosis and Hemostasis Issues in Cancer, 2026
Vol. 5 No. s1 (2026)
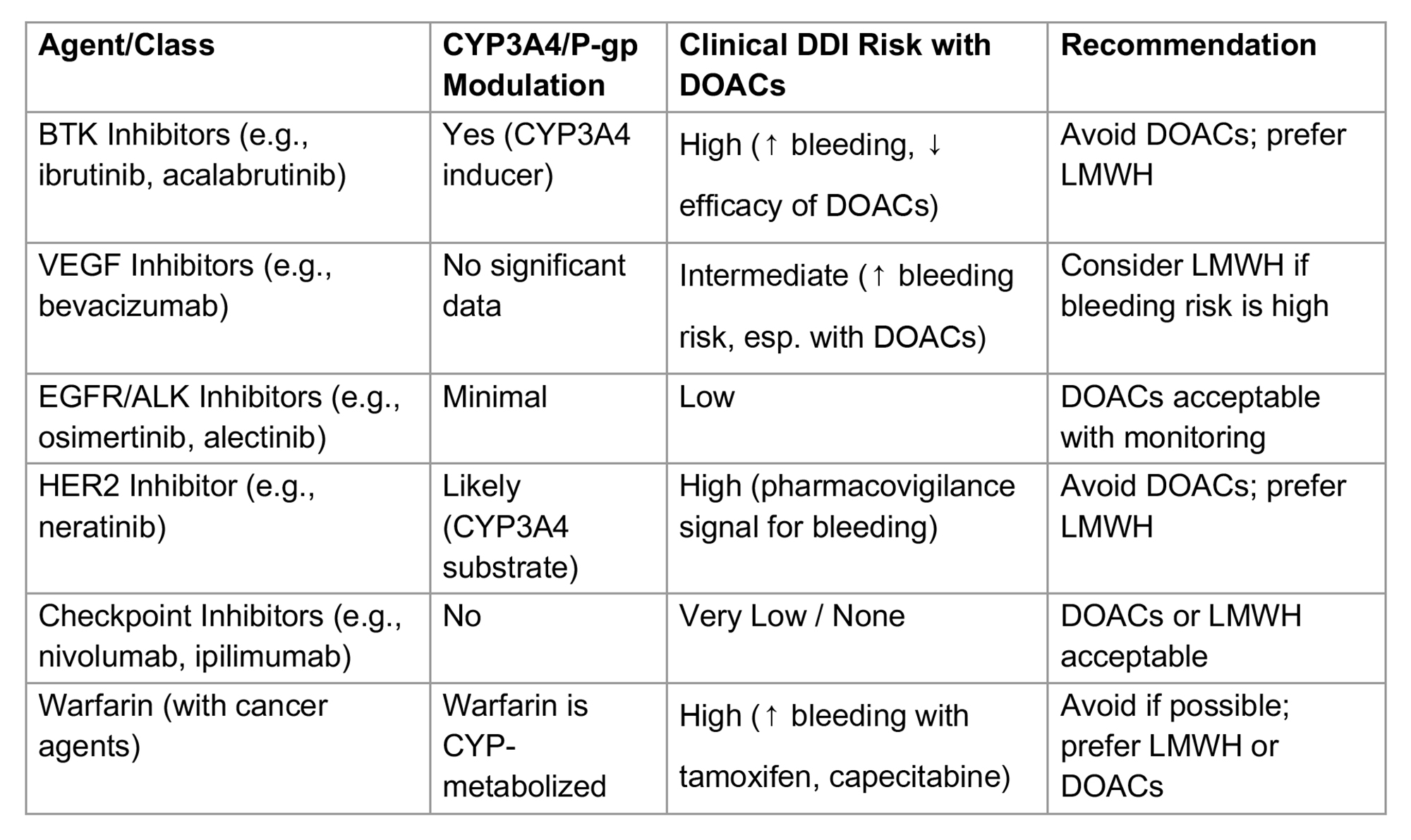
PO28 | CLINICAL IMPLICATIONS OF ANTICOAGULANT DRUG INTERACTIONS WITH TARGETED AND IMMUNE THERAPIES IN ONCOLOGY: A CONTEMPORARY RISK STRATIFICATION FRAMEWORK
D. Dhami1, C. Solowiej Singh 1, M. Dhami 2 | 1Abrazo Internal Medicine Residency; 2Eastern Connecticut Hematology Oncology, Norwich, CT, USA

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 16 April 2026
128
Views
24
Downloads
Most read articles by the same author(s)
- Società Italiana di Emostasi e Trombosi, PO49 | PROPHYLACTIC ANTICOAGULATION DECISIONS IN HIGH-RISK PATIENTS RECEIVING CANCER-DIRECTED THERAPY: ANALYSIS OF THE VERMONT METHOD , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO23 | IMMUNE THROMBOTIC THROMBOCYTOPENIC PURPURA RELATED TO DELAYED IMMUNE CHECKPOINT INHIBITORS TOXICITY: A CASE REPORT , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO69 | INCIDENTAL CANCER DETECTED DURING EMERGENCY DIAGNOSTIC WORK-UP FOR ACUTE PULMONARY EMBOLISM: A RETROSPECTIVE COHORT STUDY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO42 | DIFFERENTIAL EXPRESSION OF HEMOSTATIC BIOMARKERS ACROSS CANCER TYPE AND DISEASE STAGE: A PROSPECTIVE ANALYSIS OF 4,292 PATIENTS FROM THE HYPERCAN STUDY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO02 | SYNERGISTIC INTERACTION OF ENDOTHELIAL AND CANCER CELLS IN THE FORMATION AND STRUCTURE OF THE FIBRIN CLOT SHIELDS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO70 | HEMOSTATIC ABNORMALITIES IN A PATIENT WITH WALDENSTRÖM'S MACROGLOBULINEMIA , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO30 | LONG-TERM ANTICOAGULANT THERAPY AND PREVENTION OF RECURRENT VENOUS THROMBOEMBOLISM IN ADVANCED OVARIAN CANCER , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO64 | MANAGEMENT OF BLEEDING RISK IN PATIENTS WITH HEPATOCELLULAR CARCINOMA RECEIVING SYSTEMIC THERAPY: A SURVEY OF CLINICAL PRACTICE , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO40 | RADAR, UK-MRA MYELOMA XV - COMPARING MRD-GUIDED TREATMENT ESCALATION AND DE-ESCALATION STRATEGIES IN PATIENTS WITH NEWLY DIAGNOSED MYELOMA SUITABLE FOR STEM CELL TRANSPLANTATION: THROMBOPROPHYLAXIS SUBGROUP STUDY PROTOCOL , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO54 | CANCER-ASSOCIATED THROMBOSIS IN ASPIRIN-TREATED PATIENTS AFTER ARTERIAL THROMBOSIS: THE COMPASS-ARTECAT-ASA PROSPECTIVE COHORT STUDY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)