Abstracts of the 13th International Conference on Thrombosis and Hemostasis Issues in Cancer, 2026
Vol. 5 No. s1 (2026)
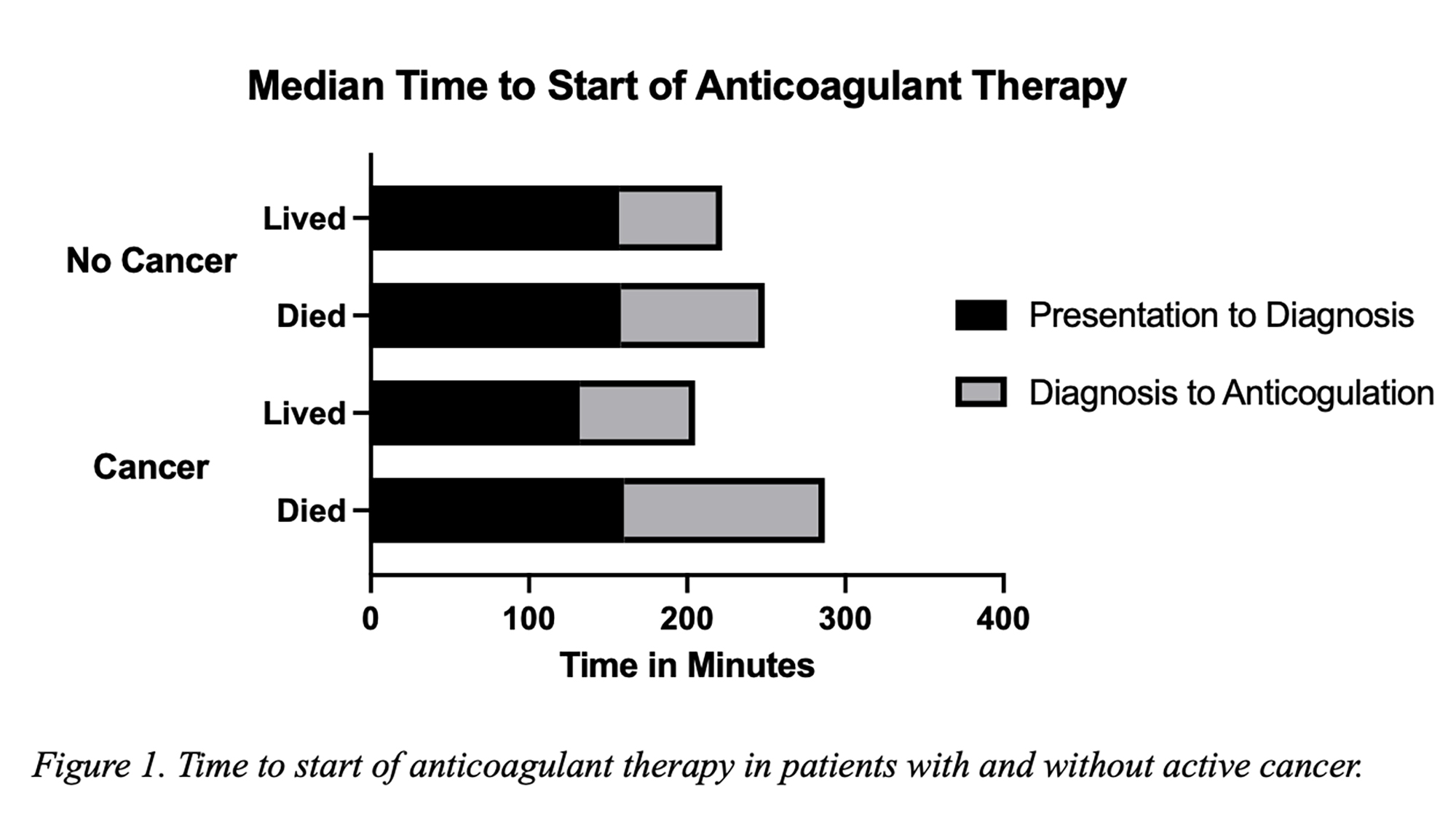
OC05 | TIME TO START OF ANTICOAGULANT THERAPY AND SURVIVAL OUTCOMES IN CANCER PATIENTS WITH PULMONARY EMBOLISM
K. Bria, B. Gage, M. Bealsey, K. Sanfilippo | Washington University in St. Louis School of Medicine, St. Louis, MO, USA

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 16 April 2026
114
Views
33
Downloads
Most read articles by the same author(s)
- Società Italiana di Emostasi e Trombosi, PO39 | RISK OF VENOUS THROMBOEMBOLISM ASSOCIATED WITH PERIPHERALLY INSERTED CENTRAL CATHETERS IN CANCER PATIENTS RECEIVING CHEMOTHERAPY: A REAL-WORLD SINGLE-CENTRE EXPERIENCE , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO32 | ANTICOAGULANT THROMBOPROPHYLAXIS IN AGGRESSIVE LYMPHOMAS PATIENTS: PREDICTIVE THROMBOTIC RISK SCORES AND RISK FACTORS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO51 | MECHANISTIC POPULATION PHARMACOKINETIC/PHARMACODYNAMIC MODELING OF FACTOR XI-TARGETING MONOCLONAL ANTIBODIES SUPPORTS DURABLE ANTICOAGULANT COVERAGE AND TRANSLATIONAL DOSE AND REGIMEN SELECTION , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO67 | TARGETED THERAPIES FOR CANCER AND THE RISK OF ARTERIAL AND VENOUS THROMBOEMBOLISM , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO09 | CANCER MORTALITY AFTER INCIDENT VENOUS THROMBOEMBOLISM , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO19 | THE INTER-RELATIONSHIP BETWEEN NETOSIS, THE ADAMTS-13/VWF AXIS, AND HEMOSTATIC ACTIVATION IN PATIENTS WITH GYNECOLOGICAL MALIGNANCIES: PROGNOSTIC SIGNIFICANCE AND IMPACT OF CHEMOTHERAPY , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO55 | HISTORY OF CANCER IN PATIENTS WITH SEVERE HEREDITARY THROMBOPHILIA VERSUS NO THROMBOPHILIA: A SINGLE-CENTER COHORT OF PATIENTS WITH VENOUS THROMBOSIS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO57 | A NOVEL RISK ASSESSMENT MODEL FOR CANCER DETECTION WITHIN ONE YEAR AFTER INCIDENT VENOUS THROMBOEMBOLISM , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, OC11 | COMPLEXITIES IN MANAGING ANTITHROMBOTIC THERAPY IN PATIENTS WITH CANCER APPROACHING END-OF-LIFE: A MIXED METHOD INTEGRATION USING JOINT DISPLAY ANALYSIS , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)
- Società Italiana di Emostasi e Trombosi, PO23 | IMMUNE THROMBOTIC THROMBOCYTOPENIC PURPURA RELATED TO DELAYED IMMUNE CHECKPOINT INHIBITORS TOXICITY: A CASE REPORT , Bleeding, Thrombosis and Vascular Biology: Vol. 5 No. s1 (2026)